Thanks to early detection and treatment, deaths due to cervical cancer have dropped in recent decades throughout most of the developed world. Yet inequitable access to screening and medical services place the mortality burden largely on the lives of women in low and middle-income countries. Every year cervical cancer claims the lives of over 200,000 women, more than 80% of whom live in the developing world, according to the World Health Organization.
Annual pap smears – which detect pre-cancerous cells that are easily treatable — are routine in wealthier nations. But pap smears are not available to the majority of women in low-income countries, which lack the laboratories and other resources required to make this early detection technique accessible to all women.
Early detection and treatment of cervical cancer is not only integral to saving lives and improving women’s overall health, it is linked to poverty reduction, education and gender equity goals. Since cervical cancer affects relatively young women – with mortality rates climbing as women enter their forties – it results in many lost years of life, delivering a devastating blow to families, communities and economies. Many of those who die are breadwinners and caretakers, leaving behind families who struggle emotionally and financially. This reduction in household income can force children – especially girls – to drop out of school in order to help provide for the family, fueling the intergenerational cycle of poverty and inequality.
The vast majority of cervical cancer cases worldwide are caused by the human papilloma virus (HPV). The virus infects the cells of the cervix and slowly causes precancerous cellular changes. Women may be infected with HPV in their teens, 20s, or 30s, but it can take as long as 20 years for the cancer to develop.
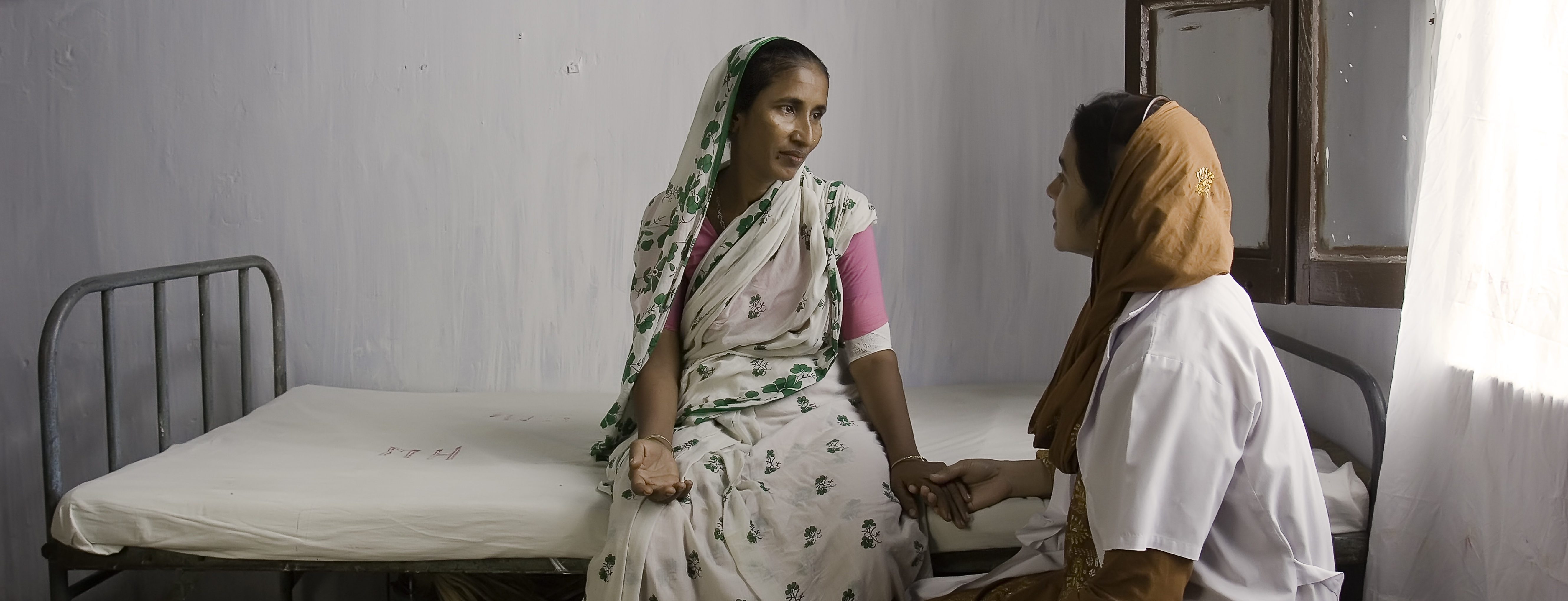
While introducing annual pap smears for all women throughout the developing world may not be possible, alternative interventions are available that can lead to the same gains wealthier nations have achieved in the battle against cervical cancer. These include: 1) adopting a cervical screening tool that is low-tech, low-cost, and effective; 2) introducing the HPV vaccine to protect girls and women against the most common cause of cervical cancer; and 3) promoting public private partnerships, such as GAVI, to help ensure an affordable, steady supply of the HPV vaccine in low-income settings.
- Adopting a simple, low-cost screening tool: The ascetic acid, or vinegar test is an effective screening technique that can be used in resource-strapped settings. Developed by a doctor in India, which has one the highest global burdens of maternal mortality, the test can be administered by a nurse or other trained healthcare worker. After applying a vinegar solution to the patient’s cervix, healthcare workers look to see whether any of the cervical area appears white, indicating follow-up testing or treatment is necessary. The test is fast, inexpensive and effective, and can be performed in the most basic health clinics, without the need for a laboratory. Based on the results of a 15-year study supported by the National Cancer Institute in the U.S., during which 150,000 women were screened, this test reduced the rate of cervical cancer death by 31%.
- Introducing the HPV vaccine into regular immunization coverage: More than 290 million women worldwide have the human papilloma virus, according to WHO, which estimates that the vaccine could prevent the deaths of over 4 million women in low- and middle-income countries over the next decade by achieving 70% coverage. While the HPV vaccine is already available as part of routine immunization regimes in 65 countries, 129 countries around the world have failed to introduce the HPV vaccine, the vast majority of them in Africa and Asia.
- Using public-private partnerships: The GAVI Alliance is one innovative public-private partnership model that is bridging the equity gap, making the HPV vaccine more affordable in low-income countries. Launched in 2000 to meet the challenges of getting vaccines out to some of the least wealthy developing countries, GAVI reached an historic agreement with vaccine manufacturers in 2013, securing a record low price for HPV vaccines. Thanks to these collaborative efforts, low-income countries can access the vaccines for as little as $4.50 per dose; by contrast, the cost in developed countries can be more than 20 times that amount. According to GAVI’s CEO, the alliance plans to reach more than 30 million girls in more than 40 countries with the vaccine by 2020.
These efforts to detect and prevent cervical cancer have the potential to save hundreds of thousands of lives. But together with the promise of such medical interventions, it is equally important to keep in mind the girls and women whom they aim to serve. Educating women about the importance of cervical cancer screening, and making steps to prevent it part of a national strategy to improve women’s health, is the most effective way to build awareness and demand for cervical cancer prevention, screening and treatment.
